What to Look for in Drug Rehab Centers

Accreditation and Clinical Standards at Drug Rehab Centers
Why Accreditation Predicts Outcomes
Checklist: Accreditation Verification
Does the rehab program have CARF or Joint Commission accreditation, and can it provide recent audit results upon request?
Accreditation acts as a critical quality signal in drug rehab centers, especially for families searching for trustworthy outcomes in regions like Oregon, Wyoming, and the broader Pacific Northwest. Accreditation means a facility has met rigorous national standards in clinical care, safety, staff training, and outcomes measurement. The most recognized accrediting bodies—such as CARF (Commission on Accreditation of Rehabilitation Facilities) and The Joint Commission—require programs to undergo thorough external audits every one to three years, verify evidence-based practices, and maintain strict documentation of client outcomes.3
Why does this matter for long-term success? These programs must demonstrate not only high-quality clinical protocols but also ongoing peer review and responsiveness to patient feedback. For worried family researchers, this translates into a reduced risk of choosing a program with outdated or non-scientific practices.
Research shows that CARF-accredited programs deliver 15-25% higher sustained recovery rates compared to non-accredited ones, making independent validation a cornerstone of effective care.3
This strategy suits organizations that want assurance a rehab center’s promises are independently validated, not just self-claimed. Accreditation also signals compliance with state requirements, which in Oregon and Wyoming means the facility is regularly inspected for safety and licensure.7
Comparison of clinical standards between accredited and non-accredited facilities.
Readers might be wondering how to check a facility’s accreditation: most reputable drug rehab centers list their status and provide documentation on request. Next, it’s worth examining how staff credentials further differentiate quality programs.
Staff Credentials That Signal Quality
Credential Assessment Tool
Does each clinical staff member hold state licensure, national certification, and specialty training in addiction treatment and mental health?
When evaluating drug rehab centers in areas like Oregon or Wyoming, staff credentials are a key signal of clinical quality. Licensed counselors and certified addiction specialists must meet state and national requirements, including ongoing continuing education and supervised clinical hours. You can often verify these licenses online; simply use Ctrl + F (or Cmd + F on Mac) to search for a specific provider's name on the state's health authority registry.
Programs in the Pacific Northwest are expected to employ multidisciplinary teams to address both substance use and co-occurring mental health needs. Look for the following credentials.7
- LPC / LCSW: Licensed Professional Counselors or Clinical Social Workers for behavioral therapy.
- CADC: Certified Alcohol and Drug Counselors specializing in substance use disorder.
- Board-Certified Physicians: Medical doctors overseeing medication-assisted treatment (MAT) protocols.
This solution fits organizations that want assurance their loved one will receive care from professionals qualified to deliver evidence-based therapies. In Oregon, the Health Authority mandates minimum staffing ratios and ongoing training—policies that directly affect treatment safety and outcomes.7
Industry leaders find that programs with highly credentialed staff see lower dropout rates and higher treatment completion, thanks to improved therapeutic alliance and better client engagement. For worried family researchers, verifying staff credentials is an essential filter: request a roster of provider qualifications and check for relevant licenses via state regulatory boards.6
Evidence-Based Treatment Modalities in Drug Rehab Centers
Behavioral Therapies That Drive Recovery
Behavioral Therapy Selection Checklist
Does the program offer Cognitive Behavioral Therapy (CBT), Motivational Interviewing (MI), and group therapy as core components, with documented outcomes?
When reviewing drug rehab centers in Oregon, Wyoming, or the broader Pacific Northwest, the evidence points strongly toward certain behavioral therapies as foundational to recovery. Cognitive Behavioral Therapy (CBT) is a structured approach that helps individuals identify and change patterns of thinking that fuel substance use. Programs that integrate Motivational Interviewing (MI)—a style that builds intrinsic motivation for change—often see improved engagement and longer retention in treatment.2
To understand how CBT is applied clinically, consider this standard thought record structure used by therapists:
Group therapy, facilitated by licensed clinicians, offers peer support and accountability, both of which research connects to higher treatment completion rates and reduced relapse risk. Opt for this framework when seeking measurable outcomes and lasting behavioral change.6
In real scenarios, programs that consistently apply these therapies see residential completion rates between 45-60%, compared to 20-30% for outpatient-only models. Prioritize this when evaluating centers in areas facing resource constraints, as structured behavioral interventions can compensate for limited specialty options. The most effective drug rehab centers not only use these therapies but also train staff in their delivery and measure client progress throughout.6

Medication-Assisted Treatment Integration
MAT Integration Decision Checklist
Does the program offer FDA-approved medications—methadone, buprenorphine, or naltrexone—alongside counseling, and employ specially credentialed prescribers?
Medication-Assisted Treatment (MAT) has become a central element in many drug rehab centers throughout Oregon, Wyoming, and the Pacific Northwest. MAT refers to the use of medications, such as methadone, buprenorphine, or naltrexone, in combination with counseling and behavioral therapies. This approach reduces cravings, stabilizes brain chemistry, and helps individuals sustain recovery, especially when facing opioid use disorder.
Research shows that MAT, when integrated into a structured program, can reduce illicit opioid use by up to 50% and improve treatment retention by 25-40% compared to counseling alone. This method works when programs have medical providers authorized to prescribe these medications and systems in place for monitoring adherence and side effects.5
For small clinics, telehealth MAT access has expanded options, particularly in rural areas. Some residential programs in the region still limit MAT use, citing philosophical differences, even though major clinical guidelines now recommend MAT as a standard of care. Consider this route if the individual’s history includes opioid dependence, chronic relapse, or unsuccessful attempts at abstinence-based treatment. The strongest outcomes occur when MAT is combined with evidence-based counseling, regular drug testing, and careful dose adjustments.2,5
Real Recovery Starts in Portland, Oregon
Call now or verify insurance to take the first step toward lasting recovery in Portland.
Co-Occurring Disorder Capabilities
Integrated Mental Health Assessment
Integrated Assessment Tool
Does the program conduct a comprehensive mental health evaluation at intake, using validated screening tools and involving licensed mental health professionals?
For drug rehab centers serving Oregon, Wyoming, and the wider Pacific Northwest, integrated mental health assessment is not just a value-add—it’s a clinical necessity. Co-occurring disorders (dual diagnosis) refer to when a person experiences both a substance use disorder and one or more mental health conditions, such as depression, anxiety, or PTSD. Studies reveal that 60-80% of individuals entering treatment have a diagnosable mental illness alongside their substance use disorder.8
It is important to note that facilities like Oregon Trail Recovery do not offer primary mental healthcare; rather, they provide specialized co-occurring mental health treatment alongside substance use disorder support. Without early, thorough assessment, these underlying issues can go unaddressed, undermining recovery outcomes.
This path makes sense for programs deploying standardized tools—like the PHQ-9 for depression or GAD-7 for anxiety—at admission, ensuring assessments are reviewed by a multidisciplinary team. Consider this method if a loved one’s symptoms suggest a history of trauma, mood instability, or self-harm. In Oregon and when utilizing Wyoming mental health resources, regulations require rehab centers to document mental health screening and coordinate integrated treatment services. While the process adds 1-3 hours to intake and requires access to licensed clinical staff, it significantly improves care matching and long-term stability.7
Trauma-Informed Care Frameworks
Trauma-Informed Care Self-Check
Does the program have written policies, staff training, and clinical protocols that address trauma history, safety, and empowerment for every participant?
Trauma-informed care is more than a buzzword—it's a treatment philosophy designed to recognize and respond to the widespread impact of trauma among people seeking help at drug rehab centers. In Oregon, Wyoming, and throughout the Pacific Northwest, programs adopting trauma-informed frameworks aim to avoid re-traumatization, foster trust, and support personal agency.
This approach is ideal for organizations supporting clients with histories of abuse, neglect, or violence, which are common among individuals with substance use disorder and co-occurring mental health conditions. Key features include:8
- Staff-wide training in trauma awareness and de-escalation.
- Safe, predictable daily routines that build a sense of security.
- Therapy models like Seeking Safety or Trauma-Focused CBT that build coping skills without forcing disclosure of painful events.
Implementation takes time: rolling out a trauma-informed framework typically requires 20-40 hours of staff training and ongoing consultation, plus updates to intake and crisis response protocols. Resource requirements may include hiring trauma specialists or contracting with consultants, depending on the organization's size.
Opt for this framework when a loved one’s symptoms involve anxiety, dissociation, or a history of adverse childhood experiences. Research shows trauma-informed approaches in drug rehab centers lead to better engagement, reduced dropout, and improved mental health outcomes for dual-diagnosis clients.8
Family Involvement and Intervention Support
Evidence-Based Intervention Models
Intervention Model Assessment Tool
Does the program offer evidence-based models like ARISE or Johnson, and provide structured support for families before, during, and after an intervention?
Evidence-based intervention models are a cornerstone for drug rehab centers in Oregon, Wyoming, and the wider Pacific Northwest—especially when a loved one resists entering treatment. The ARISE model emphasizes collaboration with the individual, using non-confrontational methods to gradually build motivation and reduce defensiveness. In contrast, the Johnson model takes a more direct approach, involving a facilitated meeting where family and friends express concerns in a unified, supportive manner.
Both models are grounded in research and can be tailored to fit a family’s dynamics, cultural background, and unique needs. This strategy suits organizations supporting families who have tried informal conversations without success or who want a structured plan to address denial or ambivalence.9
Programs offering these interventions typically require a certified interventionist, family preparation sessions, and post-intervention follow-up, amounting to 10–20 hours of professional time. Studies reveal that such models can increase treatment entry rates by 30% or more compared to unstructured attempts. As readers consider next steps, understanding how family therapy and ongoing support continue the momentum after intervention is the logical progression.9
Family Therapy and Continuing Support
Family Therapy and Support Tool
Does the program integrate regular family therapy sessions and offer structured continuing support, such as alumni groups or follow-up check-ins, to sustain engagement after treatment?
Family therapy is a core feature of quality drug rehab centers in Oregon, Wyoming, and the Pacific Northwest. Research shows that programs including family therapy boost abstinence rates by 20-30% over individual-only treatment, largely by improving communication, rebuilding trust, and helping families develop healthy boundaries. Approaches often include weekly sessions led by licensed therapists, psychoeducation for families, and skill-building for conflict resolution.6
Consider this method if families are ready to participate actively and when programs tailor support to cultural or logistical needs—such as offering virtual sessions for rural clients. For individuals requiring higher levels of initial care, Oregon Trail Recovery partners with Pacific Crest Trail Detox for residential, inpatient, or detox treatment before transitioning into intensive outpatient or sober living programs.
Continuing support is equally crucial. Effective drug rehab centers maintain engagement through alumni groups, scheduled follow-ups, or peer mentoring. These resources help prevent relapse by reinforcing accountability and providing a safe space to discuss challenges post-discharge. For organizations aiming for long-term outcomes, prioritizing robust aftercare and ongoing family involvement is key to sustaining recovery momentum.9
Your Next Steps Toward Effective Care
Finding the right treatment path starts with reaching out. For families navigating the complexities of getting a loved one into care—especially when resistance is high—professional intervention support can make all the difference. Evidence-based models like the ARISE and Johnson approaches create structured, compassionate opportunities for individuals to recognize their need for help and agree to treatment.
The next step involves connecting with a program that offers the full continuum of care. For those needing immediate medical stabilization, Oregon Trail Recovery partners with Pacific Crest Trail Detox for residential and detox services. Following detox, individuals can transition into intensive outpatient services and sober living. Gender-specific treatment tracks allow men and women to address the unique challenges they face in recovery environments designed specifically for their needs.
For Native American clients and families, culturally responsive Wellbriety programming honors traditional healing practices alongside evidence-based therapies like CBT and DBT. These specialized approaches—increasingly available across Central Oregon, Oregon addiction treatment centers, and Wyoming drug rehab facilities—recognize that effective care must address both substance use and the underlying trauma that often accompanies it.
Most insurance providers cover these services, and many facilities can facilitate admission within 24 hours once the decision is made. Families working in the behavioral health field understand that timely access matters—momentum built during intervention can quickly fade without immediate follow-through. Reaching out for a confidential consultation allows families to explore options, verify coverage, and create a coordinated plan that supports both immediate safety and long-term recovery.
Your recovery journey is unique, but you don’t have to walk it alone. Oregon Trail Recovery is here to provide the support, guidance, and evidence-based treatment you need to succeed. Take that first step today—your future self will thank you.
Frequently Asked Questions
How long should residential treatment last for optimal outcomes?
Research shows that residential treatment is most effective when it lasts at least 90 days, with programs in Oregon, Wyoming, and the Pacific Northwest typically recommending stays of three to six months for optimal outcomes. Shorter stays can lead to higher dropout rates and lower sustained recovery, especially for individuals with severe substance use disorder or co-occurring mental health needs. This approach works best when the individual requires intensive structure and has a history of relapse or unsuccessful outpatient attempts. Drug rehab centers that offer step-down care or transitional housing after residential treatment often see higher long-term recovery rates by supporting continued progress post-discharge.2
What are typical completion rates, and what factors improve retention?
Completion rates for drug rehab centers vary by setting and program structure. Residential treatment programs typically report 45-60% completion, while outpatient-only models see much lower rates, around 20-30%. Several factors help improve retention: strong peer support, consistent staff-client relationships, regular family involvement, and structured daily routines all contribute to participants staying engaged in treatment. This approach is ideal for organizations that want to maximize treatment engagement and outcomes. Research shows that programs with alumni groups or ongoing peer mentoring also see higher retention and lower dropout. Prioritizing these elements can help families support their loved one’s success.6
How do I choose between residential and intensive outpatient programs?
Choosing between residential and intensive outpatient programs depends on several clinical and logistical factors. Residential treatment provides 24/7 structure and is recommended for individuals with severe substance use disorder, unstable living environments, or repeated outpatient failures. Completion rates are higher—typically 45-60%—compared to outpatient models that average 20-30% completion. This approach works best when someone needs intensive support or has co-occurring mental health concerns that require close monitoring. Intensive outpatient programs suit those with stable housing, strong external support, and mild-to-moderate symptoms. Consider this route if daily life obligations or cost make full-time residential care impractical.4,6
What budget range should families expect for quality residential treatment?
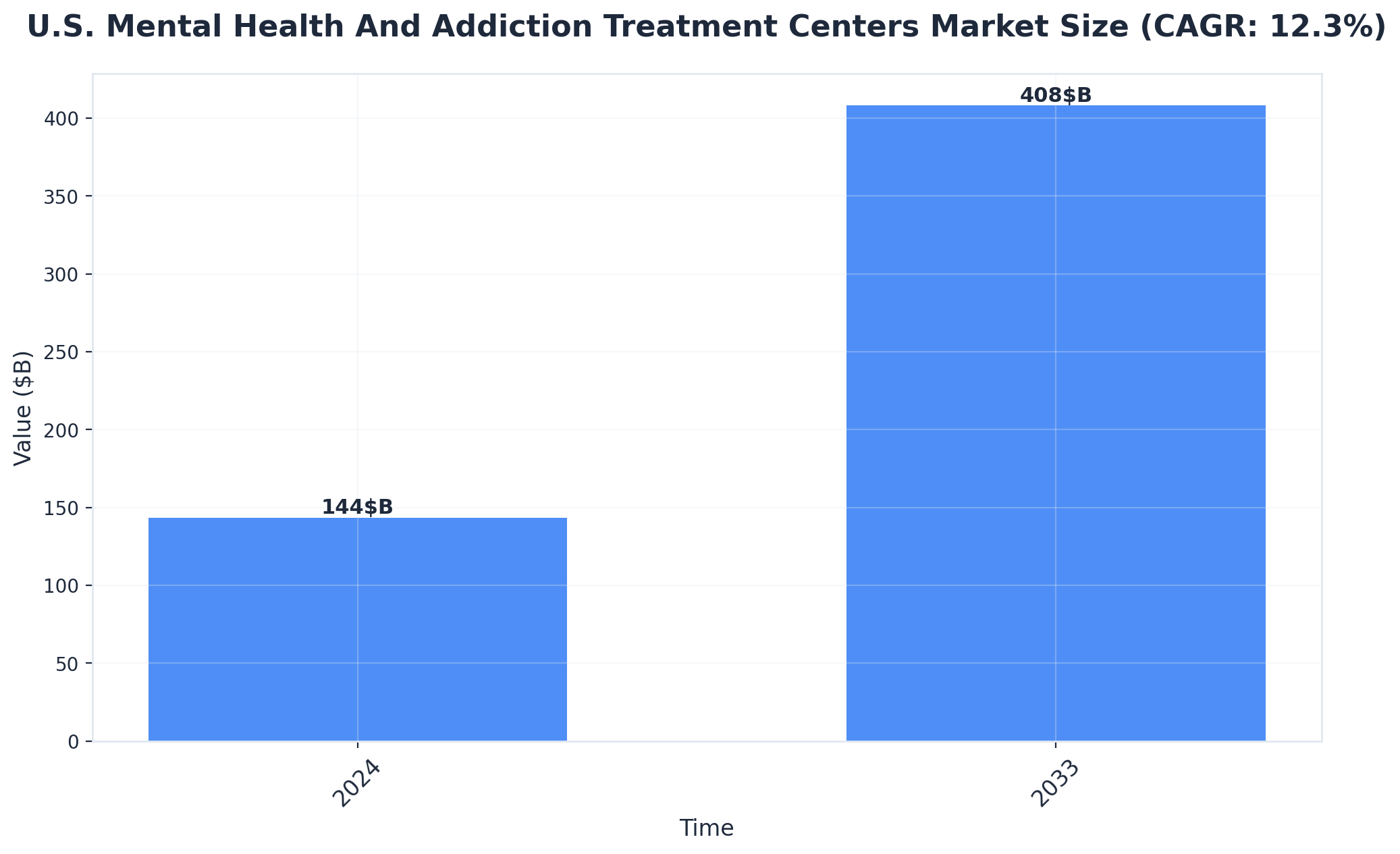
Families researching quality residential care at drug rehab centers in Oregon, Wyoming, or across the Pacific Northwest often find that costs can vary significantly depending on location, program length, and included services. While exact price points are rarely published due to insurance and privacy factors, most reputable programs charge for comprehensive care that includes medical oversight, evidence-based therapies, and family support. Industry data shows the U.S. addiction treatment market is projected to grow past $18 billion by 2025, reflecting the complexity and resource intensity of these services. Consider this route if your loved one requires 24/7 supervision and access to specialized care teams. Always verify what insurance covers and what out-of-pocket expenses to expect before committing.5
Should relapse after treatment be considered a program failure?
Relapse after treatment should not be seen as a program failure, but rather as a recognized part of the recovery process for many individuals. National research finds that relapse rates for substance use disorder mirror those of other chronic illnesses—about 40-60%—and indicate that treatment or support needs to be adjusted, not that the effort was wasted. Drug rehab centers in Oregon, Wyoming, and the Pacific Northwest increasingly emphasize relapse prevention skills and ongoing support, recognizing that recovery is a long-term journey. This approach is ideal for organizations aiming to create systems where setbacks are addressed through continued care, not blam.10
How quickly can admission occur for someone in crisis?
Admission timelines at drug rehab centers can vary, but many programs in Oregon, Wyoming, and the Pacific Northwest now offer rapid intake—sometimes within 24 hours—especially for individuals in acute crisis. The most efficient admissions occur when programs maintain on-call staff and have streamlined pre-admission assessments ready for urgent situations. Research shows that quick access reduces the risk of overdose, withdrawal complications, or dropout before treatment begins. This approach is ideal for organizations that prioritize immediate safety and are prepared to coordinate insurance verification and medical clearance quickly. Always inquire about a center’s emergency protocols and after-hours support to ensure timely entry.2
What continuing support should programs offer after residential treatment ends?
Quality drug rehab centers in Oregon, Wyoming, and the Pacific Northwest should offer structured continuing support after residential treatment. This typically includes regular alumni meetings, scheduled follow-up calls, peer mentoring, and access to support groups. Research shows that these aftercare services help maintain engagement and reduce relapse rates by providing ongoing accountability and a sense of community. This approach works best when programs customize follow-up based on individual needs, such as offering telehealth check-ins for those in remote areas. For organizations aiming for long-term recovery outcomes, robust aftercare is a key predictor of sustained success.9
References
- 2023 National Survey on Drug Use and Health (NSDUH) - SAMHSA. https://www.samhsa.gov/data/sites/default/files/reports/rpt44945/2024nsduhdetailedtabs/2024nsduhdetailedtabs.htm
- Principles of Drug Addiction Treatment: A Research-Based Guide (3rd Edition) - NIDA. https://www.nida.nih.gov/publications/principles-drug-addiction-treatment-research-based-guide-third-edition
- CARF International Accreditation Standards for Addiction Services. https://www.carf.org/Accreditation/Accreditation-Standards-Areas/Addiction-Services/
- ASAM Levels of Care and Treatment Matching - American Society of Addiction Medicine. https://www.asam.org/quality-practice/practice-standards-guidelines
- Medication-Assisted Treatment (MAT) - SAMHSA. https://www.samhsa.gov/medication-assisted-treatment/medications-counseling-behavioral-therapies
- Treatment Dropout Rates and Predictors - Journal of Substance Abuse Treatment. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5314584/
- Oregon Health Authority - Addiction and Mental Health Services Directory. https://www.oregon.gov/odhs/MCO/Pages/index.aspx
- Co-Occurring Mental Health and Substance Use Disorders - NAMI. https://www.nami.org/Get-Involved/Advocacy/Policy-Platform/SUD-and-Mental-Health-Co-Occurring-Disorders
- Family Support and Interventions - SAMHSA. https://www.samhsa.gov/treatment/family-support
- Understanding Relapse - NIDA. https://www.nida.nih.gov/publications/drugs-brains-behavior-science-addiction/relapse
Relapse Doesn't Mean the End Of Your Journey
Reach out today to explore programs that support real, long-term sobriety.







